Pump Therapy Criteria Explained: Are You Ready to Pump?

Is an Insulin Pump Right for You?
The criteria for insulin pump therapy depend on both medical need and personal readiness. While insulin pumps can dramatically improve diabetes management, they're not right for everyone. Understanding these criteria helps you make an informed decision with your healthcare team.
Key criteria include:
- Clinical need: High HbA1c (>7.0%), frequent hypoglycemia, or wide blood glucose swings despite multiple daily injections
- Personal readiness: Motivation to learn, ability to monitor blood glucose 4+ times daily, and strong problem-solving skills
- Insurance requirements: Documentation of diabetes education, 3-6 months of multiple daily injections, and detailed glucose logs
- Physical capability: Good vision and dexterity to operate the device safely
- Support system: Access to diabetes specialists and ongoing education
As one diabetes expert notes: "Insulin pump therapy gives people with diabetes the freedom to enjoy life, despite their chronic condition." But this freedom comes with responsibility.
The choice between continuing multiple daily injections (MDI) and switching to pump therapy isn't permanent. Many people successfully transition back and forth based on their changing needs and life circumstances.
Whether you're dealing with unpredictable blood sugars, frequent lows, or simply want more flexibility in your daily routine, understanding pump criteria is your first step toward better diabetes management.

Related content about criteria for insulin pump therapy:
- advantages and disadvantages of insulin pump therapy
- continuous glucose monitoring system
- how to use insulin pump therapy
The Foundation: Clinical Indications for Insulin Pump Therapy
The core criteria for insulin pump therapy are based on medical need. Your healthcare team uses these guidelines to determine if this advanced technology will truly benefit your diabetes management, especially if multiple daily injections (MDI) aren't meeting your goals.
Who is a Good Candidate from a Medical Standpoint?
An insulin pump may be recommended if you experience:
- Inadequate Glycemic Control: This is the primary reason. It includes a high HbA1c (often >7.0%) despite optimized MDI therapy, or wide, unpredictable blood sugar swings (high glycemic variability).
- Frequent or Severe Hypoglycemia: Regular low blood sugar episodes (<70 mg/dl), especially those that are severe or occur without warning (hypoglycemia unawareness), are a strong indicator for pump therapy.
- Specific Conditions: Pumps are particularly helpful for managing the dawn phenomenon (morning blood sugar spikes) and gastroparesis (slow stomach emptying). The precise insulin delivery is also crucial for women planning or during pregnancy.
- Diabetes Type: While people with Type 1 diabetes are common candidates, those with Type 2 diabetes who require complex insulin regimens and still have poor control can also benefit significantly.

Understanding Glycemic Variability
It's not just about your average blood sugar, but how much it fluctuates. Wide swings can be exhausting and dangerous. A key goal of pump therapy is to increase your Time in Range (TIR)—the percentage of time your blood sugar stays in a healthy zone.
Most insurance companies require you to try MDI therapy for a documented period (usually 3-6 months) before approving a pump. This ensures that conventional therapy has been fully optimized first. The difference in control is often visible on glucose graphs, with pump users seeing gentler hills instead of jagged peaks.
Specific Insurance and Medicare Benchmarks
Getting insurance approval involves meeting specific benchmarks. While it can feel like jumping through hoops, each requirement has a medical reason. Common requirements include:
- Documented Glucose Logs: Showing at least four blood sugar checks daily.
- HbA1c Levels: Typically two readings above 7.0% or a history of significant recurring hypoglycemia.
- C-Peptide Levels (for Medicare): A fasting C-peptide level at or below 110% of the lab's lower limit to confirm limited insulin production.
- Completed Diabetes Education: Proof of training is essential for safe and effective pump use.
- MDI Trial: A documented 3-6 month trial of multiple daily injections is usually required for those with Type 2 diabetes.
At ProMed DME, we understand these requirements and can help guide you through the approval process with your healthcare team. For more clinical details, you can reference guidance on CSII for diabetes mellitus.
Assessing Your Readiness: Essential Attributes and Lifestyle Factors
Beyond meeting medical requirements, being ready for an insulin pump is about personal commitment. The most advanced technology won't help if you're not prepared to use it effectively.
Key Personal Attributes for Pump Success
Successful pump therapy relies on your active participation. Key attributes include:
- Motivation and Realistic Expectations: You must genuinely want better control and understand that a pump is a tool that assists your efforts, not an automated cure.
- Problem-Solving Skills: You'll need to troubleshoot issues like unexpected high blood sugar or pump alarms calmly and safely.
- Technical and Physical Ability: This includes having the vision and dexterity to operate the device, change infusion sets, and hear alarms.
- Willingness to Learn: Mastering concepts like carb counting and correction factors is essential.
- Emotional Stability and a Support System: Managing diabetes can be stressful. Support from family, friends, and your healthcare team is invaluable.
- Comfort with a 24/7 Device: You must be willing to wear a device attached to your body around the clock.
How Lifestyle Impacts Your Candidacy
Your daily routine can reveal if a pump is a good fit. Pumps often work best for people whose lifestyles are challenging for traditional injection schedules.
- Active Lifestyles: A pump allows you to temporarily adjust or suspend insulin for exercise, reducing the risk of hypoglycemia.
- Erratic Schedules: Shift work or unpredictable days become more manageable with the flexibility of a pump, eliminating rigid meal and injection times.
- Frequent Travel: Adjusting to time zone changes is simpler with a pump's internal clock.
- Desire for Spontaneity: Pumps allow you to bolus for unplanned meals without disrupting your entire insulin schedule.
- Needle Phobia: Changing an infusion set every 2-3 days is often more tolerable than 4-6 daily injections.

The Commitment: Safety and Monitoring Requirements
Pump therapy requires active, engaged participation. This is not a "set it and forget it" device. Key commitments include:
- Frequent Glucose Monitoring: You must check your blood sugar at least four times daily or use a Continuous Glucose Monitor (CGM). This is your primary safety system.
- Advanced Carbohydrate Counting: Accurate carb counts are essential for the pump's bolus calculator to work correctly.
- Understanding Insulin on Board (IOB): Your pump tracks active insulin to prevent "stacking" doses, which can cause dangerous lows.
- Proper Infusion Site Care: You'll need to change your infusion set every 2-3 days and rotate sites to prevent infection and ensure good insulin absorption.
- DKA Risk Awareness: Because pumps only use rapid-acting insulin, any interruption in delivery can lead to Diabetic Ketoacidosis (DKA) quickly. You must know the warning signs and how to respond.
- Troubleshooting Skills: You will learn to identify and solve common pump issues and know when to switch to backup insulin injections.
Navigating the Technology: Pumps, CGMs, and Other Options
The world of diabetes technology is constantly evolving, but choosing the right device doesn't have to be complicated. The goal is to find the technology that best fits your lifestyle and management needs.
Understanding Different Insulin Pumps and Infusion Sets
Today's pumps are sleek and discreet. The two main types are:
- Tubed Pumps: A small device that sits in your pocket or clips to your clothing, connected to your body by a thin, flexible tube.
- Patch Pumps: A tubeless device that sticks directly to your skin.

Key features to consider include insulin reservoir capacity, the precision of basal rate increments, waterproof capabilities, and cloud connectivity for data sharing. You'll also choose an infusion set—the part that delivers insulin under your skin. Options include soft Teflon cannulas or steel needles, with different insertion angles to suit your body type. Finding the right combination may take some trial and error.
The Power of Integration: How CGM Works with Insulin Pumps
Combining an insulin pump with a Continuous Glucose Monitor (CGM) transforms diabetes management from reactive to predictive. A CGM measures your glucose levels every few minutes, giving you a real-time view of your trends.
This integration enables Automated Insulin Delivery (AID) systems, also known as hybrid closed-loop systems. These smart systems can predict where your glucose is heading and automatically adjust insulin delivery. Key features include:
- Predictive Low Glucose Suspend (PLGS): Temporarily stops insulin delivery to prevent hypoglycemia, providing peace of mind, especially overnight.
- Automatic Correction Boluses: Some systems can automatically deliver extra insulin to correct high glucose levels.
This technology represents a huge step forward, delivering insulin more intelligently based on your body's real-time needs. You can learn more about the results of these systems by reviewing the latest research on Control-IQ outcomes.
Comparing Insulin Pumps to Other Delivery Methods
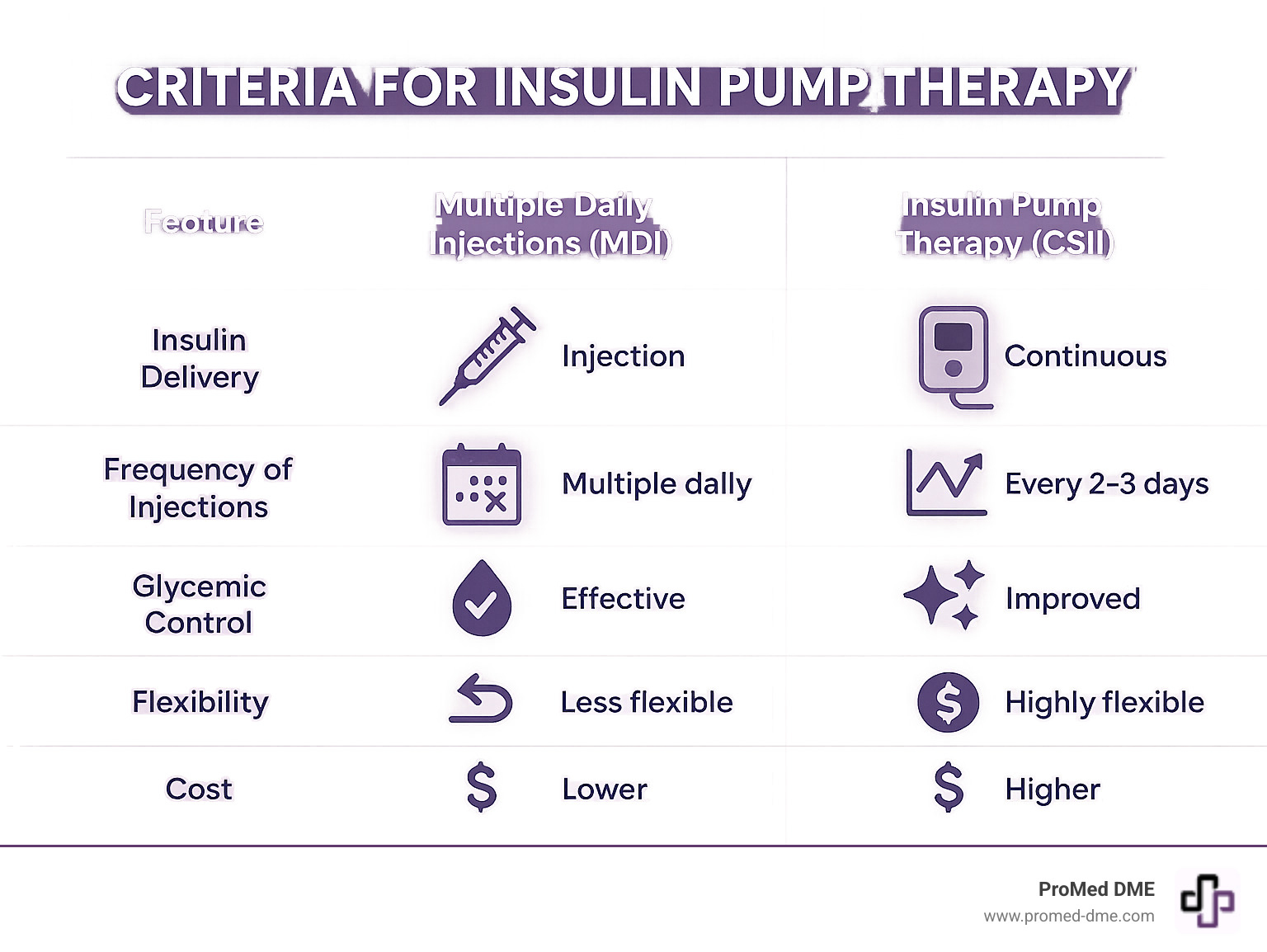
Both pumps and Multiple Daily Injections (MDI) can lead to excellent diabetes management, but pumps offer distinct advantages:
- Precision: Pumps deliver tiny, continuous amounts of rapid-acting insulin, more closely mimicking a healthy pancreas than long-acting insulin injections.
- Flexibility: With a pump, you can easily adjust for meals, exercise, or changes in your schedule without being locked into a rigid injection routine.
- Fewer Injections: You change an infusion set every 2-3 days instead of taking 4-6 injections daily.
However, pumps require more vigilance. Since they only use rapid-acting insulin, any interruption in delivery can lead to high blood sugar and potential ketoacidosis more quickly than with MDI. You must be alert to alarms and always have backup supplies.
The Practicalities: Understanding the Full Criteria for Insulin Pump Therapy
Getting approved for a pump is just the first step. The practicalities involve understanding the financial landscape, building a strong healthcare team, and preparing for the ongoing commitment.
Financial and Insurance Criteria for Insulin Pump Therapy
While pump therapy has a high initial cost, insurance can make it affordable. Here's what you need to know:
- Insurance Coverage: Most private plans cover pumps, though some may limit brand choice. Pumps are typically classified as Durable Medical Equipment (DME), meaning you pay a percentage of the cost after meeting your deductible.
- Prior Authorization: Your provider must submit documentation proving medical necessity, including glucose logs and HbA1c levels, to meet the criteria for insulin pump therapy.
- Cost: A new pump can cost up to $10,000, but your out-of-pocket expense will depend on your plan. Ongoing supplies (infusion sets, reservoirs) can cost $0 to $200 monthly after insurance.
- Medicare/Medicaid: Medicare Part B typically covers 80% of approved costs for pumps (HCPCS code E0784) after the deductible. Medicaid coverage varies by state.
- Replacement Cycle: Most insurers follow a four-year replacement cycle, aligning with pump warranties.
At ProMed DME, we work with most insurance plans and handle the verification process to help you understand your costs upfront. For more details, see these Diabetes Tech Billing Codes & Reimbursement guidelines.
The Role of Your Healthcare Team
Successful pump therapy is a team sport. Your team includes:
- Endocrinologist/Diabetes Specialist: Prescribes the pump and manages your overall care.
- Diabetes Care and Education Specialist (DCES): Provides comprehensive training on pump use, carb counting, and troubleshooting. You can find one using the ADCES finder tool.
- Pump Trainer: Provides hands-on education for your specific pump model.
- Registered Dietitian: Helps you master advanced carbohydrate counting.
Ongoing follow-up with this team is crucial for long-term success and is often required by insurance.
Special Considerations and Criteria for Insulin Pump Therapy
Certain situations require special attention:
- Pediatric Patients: Approval criteria may be more flexible, but caregiver involvement is critical. The caregiver must be able and willing to manage the pump safely.
- Discontinuation: Pump therapy can be discontinued if it's no longer the right choice due to changes in health, ability, or personal preference. This is not a failure, but a change in treatment plan.
- Potential Challenges: Be aware of risks like infusion site infections and high blood sugar from delivery interruptions. Your healthcare team will prepare you to handle these issues.
Frequently Asked Questions about Insulin Pump Criteria
We know you probably have more questions about whether an insulin pump might be right for you. These are some of the most common questions we hear about the criteria for insulin pump therapy:
What is the main reason someone gets approved for an insulin pump?
The primary reason is a documented clinical need that isn't being met by multiple daily injections (MDI). This often includes:
- Frequent or severe hypoglycemia (low blood sugar), especially if it's unpredictable or occurs without warning.
- Persistently high HbA1c levels (usually above 7.0%) despite actively managing diabetes with MDI.
- High glycemic variability (wild blood sugar swings).
Your provider must document that you've given MDI a fair trial (usually 3-6 months) to prove a pump is medically necessary for your health and safety.
Is using an insulin pump a lifelong commitment?
No, it is not a lifelong commitment. It's a flexible treatment tool. Many people use pumps continuously, but others take "pump holidays" or switch back to injections for periods. This is a personal choice made in consultation with your healthcare team to ensure your blood sugars remain stable during any transition.
How much does an insulin pump cost with insurance?
The cost varies widely based on your insurance plan. Most pumps are covered as Durable Medical Equipment (DME), meaning you'll likely pay a percentage of the cost after meeting your deductible. For example, Medicare Part B typically covers 80% of the approved amount.
The pump itself can have a list price of over $9,000, but your out-of-pocket cost will be much lower. Ongoing supplies like infusion sets and reservoirs also have associated costs, which depend on your plan's DME or pharmacy benefits.
Insurers typically cover a new pump every four years. Our team at ProMed DME works with most insurance plans to verify your benefits and help you understand your potential costs upfront.
Conclusion: Taking the Next Step in Your Diabetes Journey
Understanding the criteria for insulin pump therapy is the first step in a potentially life-changing journey. The decision to use a pump is a partnership between you and your healthcare team, based on your clinical needs, lifestyle, and personal readiness.
Whether you're struggling with blood sugar swings, seeking more flexibility, or concerned about hypoglycemia, you have options. Modern diabetes technology offers a level of control and freedom that was once unimaginable.
The criteria we've discussed are guideposts to help ensure you're set up for success. While your healthcare team determines if you meet the clinical requirements, only you can decide if you're ready for the commitment.
At ProMed DME, we understand that navigating insurance and costs can be overwhelming. Our team works with most insurance plans to minimize your out-of-pocket expenses. We have a dedicated nurse on staff to answer your questions and offer support. From initial insurance verification to ongoing supply deliveries with free shipping, we are committed to making this process as smooth as possible.
If you're ready to explore whether pump therapy is right for you, talk to your endocrinologist. Share your goals and frustrations, and ask about your options. Your diabetes journey is yours, but you don't have to steer it alone.
Related Resources & Articles
Stay informed with our informative blog posts.
Discover the ProMed Advantage
& Try Our Products
We offer free shipping and legendary customer service to ensure you receive the
best DME products for your needs.