Detailed Guide to Choosing Wound Dressings for Burns
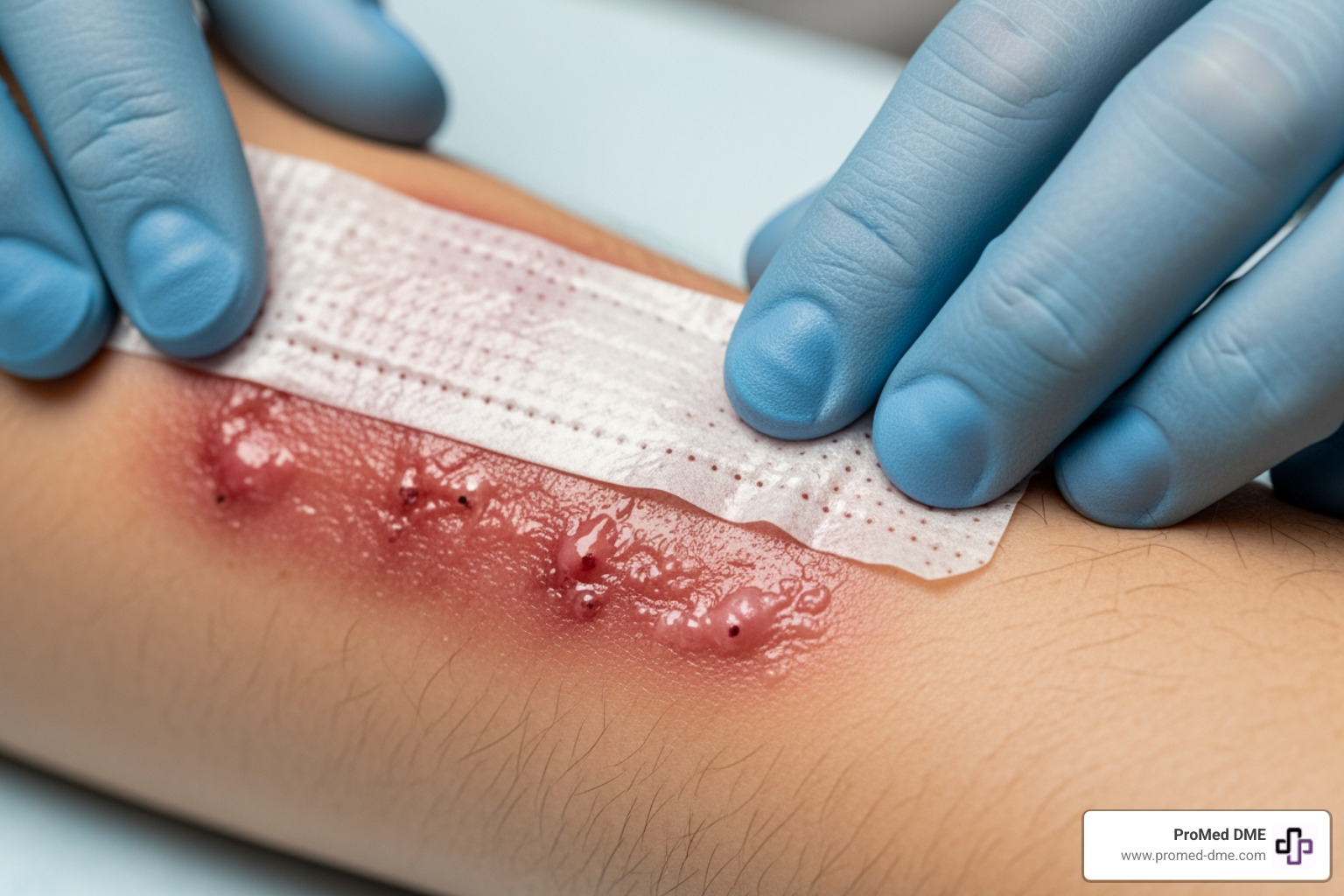
Understanding Burn Injuries and the Importance of Proper Wound Care

Wound dressing for burns is a critical component of the healing process that can significantly impact recovery time, reduce infection risk, and minimize scarring. Whether you're managing a minor kitchen accident or a more serious injury, selecting the right dressing makes all the difference in how well and how quickly your skin heals.
Quick Answer: Best Wound Dressings for Burns by Type
| Burn Depth | Recommended Dressing | Key Benefits |
|---|---|---|
| Superficial (1st degree) | Moisturizer only, no dressing needed | Keeps skin hydrated during healing |
| Superficial partial-thickness (2nd degree) | Hydrocolloid or silver-impregnated dressings | Maintains moisture, reduces infection risk, fewer changes |
| Deep partial-thickness | Foam, alginate, or biosynthetic dressings | Manages high exudate, promotes faster healing |
| Full-thickness (3rd degree) | Requires medical intervention and specialized coverage | Protects wound bed until surgical treatment |
In the United States, chronic wounds, including burns, contribute to more than $25 billion in healthcare costs annually, highlighting why proper wound care is so important.
The right wound dressing does more than cover an injury. It creates an optimal healing environment by maintaining moisture, preventing infection, reducing pain, and protecting the wound bed. Research shows that wounds healing within two weeks typically leave minimal scarring, while those taking longer often result in more noticeable scars. Your choice of dressing can directly influence this outcome.
This guide will help you understand the different types of burn wound dressings, when to use them, and how to care for your burn at home. We'll cover everything from first aid to long-term scar prevention to help you make informed decisions about your recovery.

First Steps: Assessing the Burn and When to Seek Medical Help
The moment a burn happens, quick decisions are crucial. Understanding the severity of the burn helps you get the right care fast.
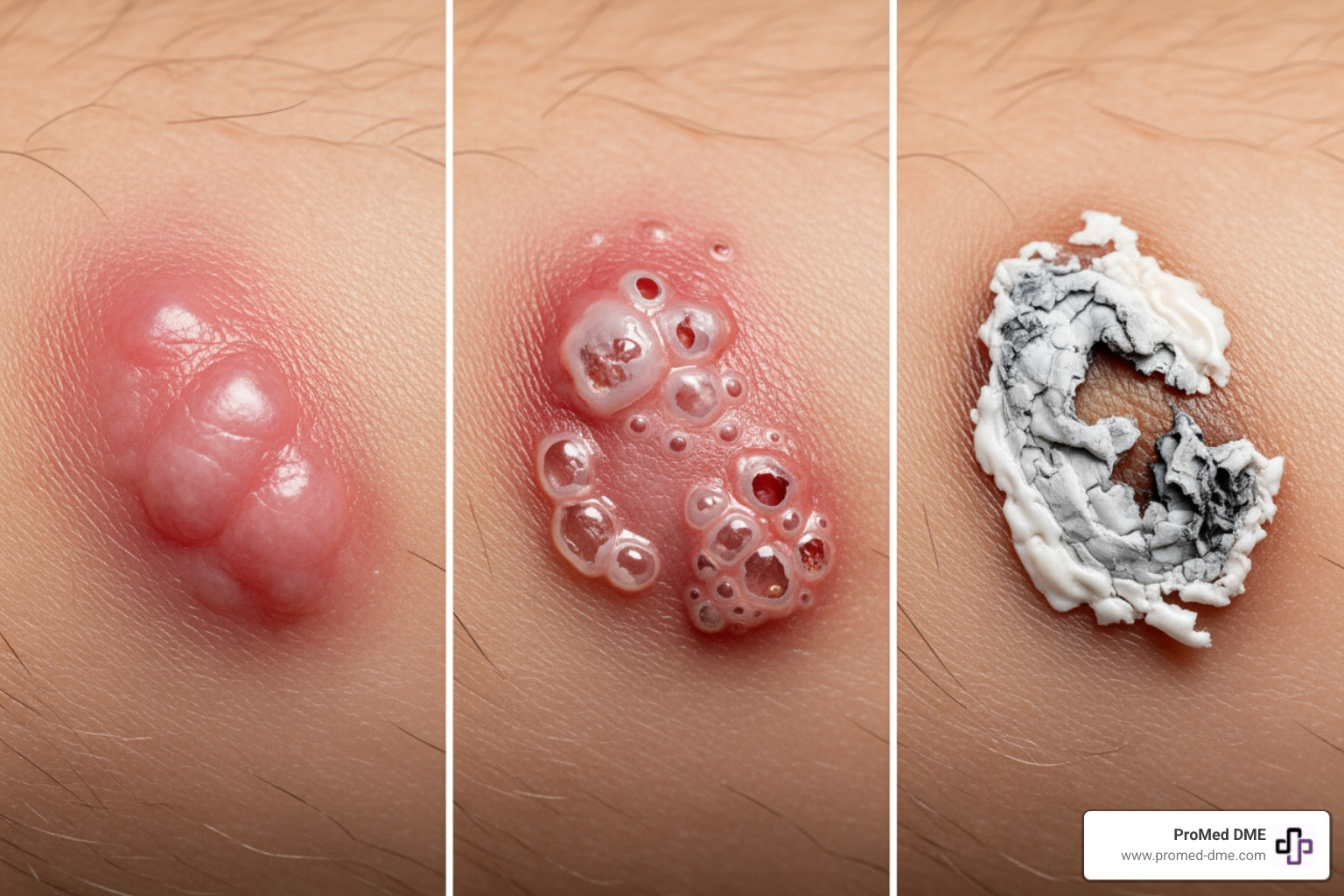
What are the different types of burns and scalds, and how are they classified?
Burns are classified by how deeply they damage the skin.
- First-degree burns affect only the outer skin layer (epidermis). The skin is red, tender, and may swell slightly, but there are no blisters. They usually heal within a week without scarring.
- Second-degree burns (partial-thickness) penetrate the second skin layer (dermis). These are where wound dressing for burns becomes vital. They are painful, red, and form blisters. Superficial ones heal in about two weeks with minimal scarring, while deeper ones take longer and may leave noticeable scars.
- Third-degree burns (full-thickness) destroy both skin layers and may extend into fat or muscle. The area may look white, black, or charred and feel leathery. These burns often don't hurt because nerves are destroyed. They always require immediate medical intervention.
A burn is from dry heat (fire, hot metal), while a scald is from wet heat (steam, hot liquid). Both are treated the same way.
What are the immediate first aid steps for burns and scalds?
What you do in the first few minutes can dramatically change the outcome.
- Cool the burn immediately. Hold the area under cool (not cold) running water for at least 20 minutes. Do this as soon as possible (within three hours of injury). This reduces pain, swelling, and can prevent the burn from deepening. Never use ice.
- Remove jewelry and tight clothing from the burned area before it swells. If clothing is stuck to the burn, leave it for medical professionals to remove.
- Cover the burn with a clean, non-fluffy cloth or plastic wrap (cling film) to protect it. Do not apply butter, oils, or creams, as they can trap heat and worsen the injury.
- Manage pain with over-the-counter pain relievers like paracetamol or ibuprofen if needed.
When should a burn or scald seek medical attention?
While many minor burns can be treated at home, seek professional medical attention immediately if:
- The burn is larger than the injured person's palm.
- The burn is on the face, hands, feet, genitals, or over a major joint.
- The burn causes blisters or appears white, black, or leathery (indicating a second or third-degree burn).
- It is a chemical or electrical burn.
- The injured person is a baby, young child, or elderly.
- There are signs of inhalation injury (coughing, hoarseness, difficulty breathing).
- You see signs of infection, such as increasing pain, spreading redness, fever, or foul-smelling drainage.
- The pain is severe and not managed by over-the-counter medication.
When in doubt, always err on the side of caution and seek professional guidance.
A Comprehensive Guide to Wound Dressing for Burns
The wound dressing for burns you choose creates the environment for your body to heal. The goals are to promote healing, prevent infection, reduce pain, and minimize scarring. An ideal dressing maintains a moist environment, protects against bacteria, and can be changed without causing more pain.
| Dressing Type | Properties | Best Use for Burns | Typical Change Frequency |
|---|---|---|---|
| Hydrocolloid | Self-adhesive, forms gel, waterproof barrier, reduces pain | Low to moderate exudate, superficial partial-thickness burns | Every 3-7 days |
| Alginate | Seaweed-derived, highly absorbent, forms gel, biodegradable | Moderate to high exudate, deep partial-thickness burns, wounds with some bleeding | Daily to every 3 days |
| Foam | Highly absorbent, cushioning, non-adherent options, thermal insulation | Moderate to high exudate, provides protection and comfort | Every 1-5 days |
| Hydrogel | High water content, soothing, cooling, donates moisture, helps debride | Dry wounds, painful burns, to soften slough/eschar | Daily |
| Silver-Impregnated | Broad-spectrum antimicrobial, sustained silver release | Burns at risk of infection or with signs of infection, partial-thickness burns | Every 1-7 days (product dependent) |
Understanding Different Types of Wound Dressing for Burns
Understanding the most common types of wound dressing for burns will help you and your healthcare provider make the best choice for your injury.
Hydrocolloid Dressings
These versatile, self-adhesive, and waterproof dressings form a gel over the wound to create a moist healing environment. They are excellent for superficial partial-thickness burns with low to moderate drainage. Studies show they can speed up healing, reduce pain, and require far fewer dressing changes than traditional methods.
Alginate Dressings
Derived from seaweed, these highly absorbent dressings are ideal for burns with moderate to high drainage. They form a gel that maintains moisture while managing excess fluid. Alginates are biodegradable and require a secondary dressing to hold them in place.
Foam Dressings
Foam dressings are highly absorbent and provide cushioning and protection, making them excellent for moderate to highly draining burns. Many have a non-adherent layer to prevent sticking to the wound, which makes changes more comfortable.
Hydrogel Dressings
With a high water content, hydrogel dressings offer a soothing, cooling effect on painful burns. They donate moisture, making them ideal for dry or sloughy burns that need rehydrating to help the body clear away dead tissue. Research in "Progress in Hydrogels for Skin Wound Repair" highlights their role in promoting cell migration to close the wound.
The Role of Antimicrobials in Wound Dressing for Burns
Preventing infection is critical. Antimicrobial dressings reduce bacteria in the wound to minimize infection risk.
Silver-Impregnated Dressings
Silver dressings release silver ions to fight a broad range of bacteria. Nanocrystalline silver technology offers a sustained release for prolonged protection. A systematic review of silver-containing dressings confirms their effectiveness for burns at risk of infection.
Honey-Based Dressings
Medical-grade honey dressings use honey's natural antimicrobial and anti-inflammatory properties. They promote a moist healing environment, help remove dead tissue, and can reduce wound odor.
Chlorhexidine Dressings
These medicated gauzes have antiseptic properties and are used for superficial burns. However, they may not be ideal for deeper wounds, as some research suggests they can be toxic to new skin cells.
Biosynthetic and Skin Substitute Dressings
For deeper or more complex burns, specialist burn centers may use biosynthetic dressings or temporary skin substitutes. These advanced dressings act as a "second skin," adhering to the wound to protect it. They dramatically reduce pain, minimize dressing changes, and promote faster, more organized healing with better outcomes. While typically used for more serious injuries in a clinical setting, they represent the cutting edge of burn care.
At ProMed DME, we understand that navigating wound care options can feel overwhelming. Our dedicated nurse is available to help answer your questions about which dressings might be right for your specific situation, and we work with most insurance plans to make quality wound care supplies accessible and affordable.
Home Care: Dressing Changes, Recovery, and Long-Term Skin Health
Proper home care is essential for a smooth recovery. Attention to dressing changes, nutrition, and long-term skin protection will make a significant difference in your healing outcome.

What are the key considerations for dressing changes and wound care at home?
Proper technique is key for preventing infection and promoting healing.
- Prepare: Gather your new sterile wound dressing for burns, mild soap, clean water, and medical tape.
- Wash Hands: Always wash your hands thoroughly before and after touching the wound.
- Manage Pain: If needed, take pain medication 30 minutes before a dressing change.
- Remove Gently: Soak a stuck dressing with warm water to loosen it before removing.
- Clean Wound: Gently clean the area with mild soap and lukewarm water, then pat dry with a clean towel. Do not rub.
- Apply New Dressing: Handle the new dressing by its edges. If using ointment, apply it to the dressing, not the wound.
- Secure: Secure the dressing so it's snug but not tight.
How does nutrition play a role in burn recovery?
Your body needs fuel to heal. Focus on a diet rich in protein (lean meats, eggs, beans) to repair tissue, and stay well-hydrated by drinking plenty of water. Vitamins A, C, and D, along with zinc, are also crucial for skin regeneration and immune function.
What are the long-term care considerations for healed burn skin, including sun protection?
Your work isn't finished when the wound closes. Newly healed skin is fragile and needs special care.
- Moisturize: Apply unscented moisturizer several times a day to combat dryness and itching. Gently massaging the area can help with scar formation.
- Manage Itching: In addition to moisturizing, wear loose, breathable clothing and keep fingernails short.
- Protect from the Sun: This is critical. Healed burn skin is extremely sensitive to the sun. For at least two years, cover the area with protective clothing and use a high-factor sunscreen (SPF 30 or higher) on all exposed healed skin.
What are the signs and symptoms that indicate a need for further medical advice after initial burn treatment?
Contact your healthcare provider immediately if you notice:
- Worsening pain, increased redness, warmth, or swelling.
- Foul-smelling or discolored drainage (pus).
- A fever of 100.4°F (38°C) or higher.
- A dressing that becomes soaked with fluid.
- Changes in circulation, such as a limb turning pale, bluish, or cold.
At ProMed DME, we understand that wound care can feel overwhelming, especially when you're managing it at home. That's why we offer a comprehensive range of wound care supplies and have a dedicated nurse on staff to answer your questions. We're here to support your healing journey every step of the way.
What is the role of specialist burn care services and potential surgical interventions like skin grafts?
Deep partial-thickness and full-thickness burns often require specialist care. This may involve surgical debridement (removal of dead tissue) followed by a skin graft. A skin graft involves transplanting healthy skin from a donor site on your body to cover the burn. This procedure is the standard for closing deep wounds that cannot heal on their own. Following surgery, long-term rehabilitation with physical and occupational therapists is crucial for maintaining joint mobility, managing scars, and preserving function.
Frequently Asked Questions about Burn Dressings
Here are answers to some of the most common questions about managing burns at home.
Should I pop a burn blister?
No, do not pop blisters at home. A blister is your body's natural, sterile wound dressing for burns, protecting the healing skin underneath from infection. Popping it creates an open wound.
A healthcare professional may decide to safely drain or remove a large, painful, or likely-to-burst blister in a clinical setting. If a blister is causing significant discomfort, seek medical advice instead of managing it yourself.
How often should I change a burn dressing?
The frequency depends on the type of wound dressing for burns and the amount of drainage.
- Traditional dressings and some creams may require daily changes.
- Modern dressings like hydrocolloids or foams can often be left in place for several days, reducing painful changes and disruption to the wound.
Always follow your healthcare provider's specific instructions. They will give you a schedule based on your specific burn. Contact them if a dressing becomes soaked, leaks, or comes loose.
What is the difference between a burn and a scald?
While the terms are often used interchangeably, there is a technical difference.
- A burn is caused by dry heat (fire, hot metal, electricity).
- A scald is caused by wet heat (steam, hot liquids).
The cause is different, but the skin damage and first aid treatment are identical for both. The most important thing is to assess the severity and get the right care.
Conclusion: Your Path to Effective Burn Recovery
Recovering from a burn injury involves understanding what your body needs to heal. From initial assessment and first aid to choosing the right wound dressing for burns, the steps you take can significantly influence your recovery.
Modern dressings like hydrocolloids and silver-impregnated products offer faster healing, less pain, and better infection prevention than older methods. Selecting the correct dressing creates the ideal environment for your skin to rebuild itself, which can lead to better cosmetic outcomes.
At ProMed DME, we are committed to supporting your recovery. Dealing with a burn is stressful enough without worrying about supplies. We offer free shipping across the United States, have a dedicated nurse on staff to answer your questions, and work with most insurance plans to minimize your costs. We provide the tools and support to help you heal.
Ready to take the next step in your healing journey? Explore more information about our wound care supplies and find how ProMed DME can support you with quality products and expert guidance. We're here to help you heal better and with confidence.
Related Resources & Articles
Stay informed with our informative blog posts.
Discover the ProMed Advantage
& Try Our Products
We offer free shipping and legendary customer service to ensure you receive the
best DME products for your needs.


